Man With Facial Plethora and Edema
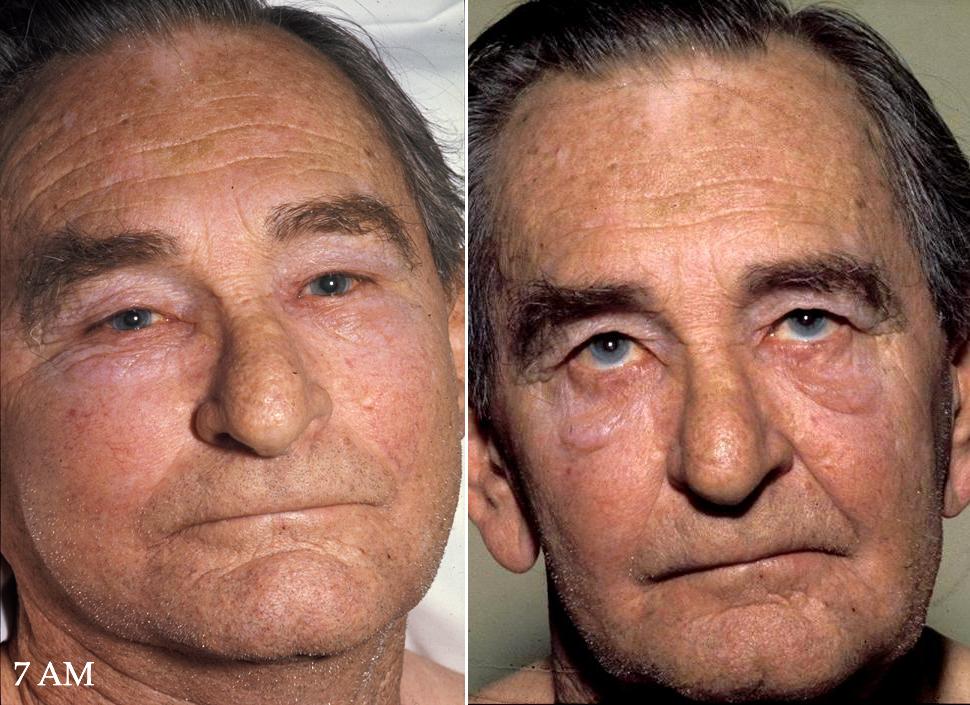
A 61-year-elderly person gives enlarging and staining of his facial plethora and neck of half a month’s length. He noted snugness of his shirt and tie, which has deteriorated. Loved ones have remarked on his appearance and have gotten some information about his condition of wellbeing. He has had no aggravation or changes in mentation, and he has had the option to play out his regular occupation as a vehicle sales rep.
HISTORY
He is a long-lasting, weighty cigarette smoker with a persistent “smoker’s hack” that probably has deteriorated as of late. He denies dyspnea on effort, however on cautious addressing he uncovers that he does to be sure experience windedness with exertion. There are no nighttime manifestations.
Actual EXAMINATION
The patient has a to some degree plethoric face. Breath rate is 20 breaths each moment; pulse, 100 beats each moment; and circulatory strain, 140/80 mm Hg. His neck and face appear to be enlarged, and the veins of his neck are widened. There are venous securities across the two facial plethora shoulders. No gross hubs are discernible in his neck or supraclavicular fossae. Heart is ordinary. Wheezes and rhonchi are heard in the lung fields, however no stridor is valued.
IMAGING RESULTS
A chest radiograph uncovers an enlarged mediastinum with likely paratracheal and hilar adenopathy on the right side.
Which of the accompanying assertions about this patient is right?
A. Any biopsy strategy ought to anticipate intense administration of his introducing disorder.
B. He ought to have stent position emanantly.
C. There is a generally 50:50 possibility that the reason for his manifestations is harmless.
D. His introducing condition won’t influence his endurance anticipation.
Right Answer: D
This present patient’s set of experiences and actual discoveries are common of the predominant vena cava (SVC) disorder, a star grouping of discoveries that outcome from some type facial plethora of blockage or pressure of the SVC as blood is gotten back to the heart. The check blocks blood stream and prompts chest area edema and over the long run the development of securities across the chest area divider as was show in this quiet. In intense circumstances, aviation route edema and cerebral edema with hazardous impacts can happen; nonetheless, target appraisal of an enormous collection of involvement shows such circumstances are very extraordinary (or really uncommon) impacts of SVC condition. Consequently, this disorder isn’t the critical crisis it was once thought to be in past decades1 and, as will be additionally talked about, there is the ideal opportunity for precise analysis and authoritative arranging of care.
ETIOLOGY
The etiology of SVC disorder has significantly changed in the course of recent years from a harmless causation (eg, tuberculosis, syphilitic aortitis) to a 90% threatening etiology (eg, cellular breakdowns in the lungs, lymphoma) to a current 2:1 proportion of dangerous to harmless because of the approach of focal venous catheters, which presently represent practically all of the harmless causation.2 Catheter etiology is generally clear by the presence of a catheter and additionally a new history of catheterization. The favored imaging concentrate in facial plethora SVC condition, CT filtering with contrast, will affirm either characteristic thrombotic impediment or extraneous neoplastic pressure to handily separate between the two. Since this patient has no set of experiences of catheter position, the probability of harm is exceptionally high and decision C isn’t right.
Determination
This prompts the subsequent stage in the assessment—making a conclusive determination. Once more, more seasoned legend has respected more present day, precise information. Fears of complexities, for example, raised venous strain actuated draining and differentiation responses are unwarranted, and fitting demonstrative methods can and ought to be utilized to rapidly make an exact diagnosis.3,4 Thus, contingent upon the clinical discoveries, bronchoscopy, lymph hub biopsy, and mediastinoscopy can and ought to be utilized to get tissue and show up at an authoritative determination. Decision An is consequently erroneous.
Yields for bronchoscopy with or without transthoracic needle biopsy are in the half to 75% territory, and mediastinoscopy procedures have yields in the 90% range.3
The executives
Authoritative administration, obviously, relies upon the particular finding. Neoplasms like little cell cellular breakdown in the lungs and lymphoma are impeccably touchy to chemotherapy, and fundamental chemotherapy will rapidly bring about goal of SVC disorder; while other strong growths normally require radiation treatment as well.1,5 In uncommon instances of extreme perilous aviation route or cerebral indications (most as often as possible when a huge occlusive apoplexy from a catheter is the reason), intravascular stenting to sidestep the deterrent can be performed.6 This is exceptional.
This patient has a subacute beginning, doesn’t have dangerous side effects or signs, has as of now created pledges, and along these lines doesn’t seem, by all accounts, to be a stent applicant, surely in a pressing setting, settling on decision B inaccurate. Maybe, he ought to have a deliberate way to deal with brief finding; mediastinoscopy would appear to accommodate his side effects and history that propose cellular breakdown in the lungs, just as his chest radiograph that shows an augmented mediastinum. Curiously and significantly, a definitive guess in instances of SVC disorder is infrequently identified with the actual condition. This difficulty quite often implies progressed sickness, yet the anticipation doesn’t seem to vary from endurance among patients with a similar cancer type and stage who don’t have SVC disorder; hence, decision D is the right assertion here.1,5
Result OF THIS CASE
A mediastinal biopsy methodology was performed without occurrence and uncovered a non–little cell carcinoma of the lung. Blend radiation and chemotherapy was started, and inside the space of weeks clinical improvement in the SVC condition discoveries came about. The conclusive treatment for the cellular breakdown in the lungs is progressing.